
When you hit your 60s, 70s, or beyond, your body doesn’t just slow down - it starts to reconfigure how it handles medications. What once worked perfectly at 40 might now make you dizzy, confused, or even end up in the hospital. This isn’t about being weak or old. It’s about biology. Specifically, how your liver and kidneys change - and what that means for every pill you take.
Why Your Liver Slows Down
Your liver is your body’s main drug-processing plant. It breaks down medicines so they can be eliminated. But after age 65, liver blood flow drops by about 40%. Liver mass shrinks by roughly 30%. These aren’t minor tweaks - they’re major shifts in how drugs get processed. Think of it like a factory with fewer workers and slower conveyor belts. Drugs that used to be cleared quickly now linger. This is especially true for drugs like propranolol, lidocaine, and morphine. These are called flow-limited drugs, meaning their clearance depends mostly on how much blood reaches the liver. With 40% less blood flow, their clearance drops by nearly the same amount. That means higher drug levels in your blood - and a higher chance of side effects like low blood pressure, dizziness, or slowed breathing. Even more surprising: some drugs become more potent because they’re absorbed better. Many pills are designed to be broken down by the liver before they enter your bloodstream - a process called first-pass metabolism. As liver function declines, less of the drug gets destroyed on the first pass. So more of it enters your system. For drugs like verapamil or propranolol, this can mean 25-50% more drug in your blood than expected. A standard dose might suddenly feel like a double dose.What Happens to Kidneys
Your kidneys filter waste - including drugs - from your blood. Between ages 30 and 80, your glomerular filtration rate (GFR) drops by 30-50%. That’s not just a number. It means your kidneys are filtering significantly less blood every minute. Here’s the catch: many older adults don’t realize this is happening. Why? Because serum creatinine - the standard blood test doctors use to check kidney function - often stays normal. That’s because muscle mass declines with age, and creatinine is made by muscle. Less muscle = less creatinine = falsely reassuring numbers. So a doctor might think your kidneys are fine when they’re actually working at 60% capacity. Drugs that leave the body mostly through the kidneys - like digoxin, lithium, or metformin - need lower doses. Too much of these can build up and cause toxicity. Digoxin overdose, for example, can cause dangerous heart rhythms. Lithium can lead to tremors, confusion, or seizures. Metformin, while generally safe, can cause lactic acidosis if kidney function drops too low. And here’s a newer finding: when kidneys fail, the liver can suffer too. Studies now show that kidney impairment reduces the activity of liver enzymes like CYP3A4. So even drugs that are processed by the liver might not be cleared properly - not because the liver is weak, but because the kidneys are. It’s a chain reaction.Phase I vs. Phase II: Not All Drugs Are Created Equal
Not every drug is affected the same way. There are two main ways the liver breaks down drugs: Phase I and Phase II metabolism. Phase I uses enzymes like CYP3A4 and CYP2D6 to modify drugs. This is where things get messy. Some studies show these enzymes decline by 37-60% in older adults - especially in animal models. But human data tells a different story. For many common drugs, like diazepam or phenytoin, Phase I activity stays relatively stable. Why? Because the liver’s enzyme quantity doesn’t drop as much as we thought. The real issue is blood flow and liver mass, not enzyme loss. Phase II metabolism - which adds molecules to drugs to make them water-soluble for excretion - holds up even better. Processes like glucuronidation (used by acetaminophen and many painkillers) don’t decline significantly with age. That’s good news. It means drugs relying on Phase II are often safer for older adults. But here’s the trap: prodrugs. These are inactive compounds that need to be converted into active drugs by the liver. Examples include perindopril (an ACE inhibitor) and codeine (which turns into morphine). If liver function drops, the conversion slows. So you might not get the full benefit - and your doctor might keep increasing the dose, thinking it’s not working. Meanwhile, you’re building up the inactive form, which can cause side effects.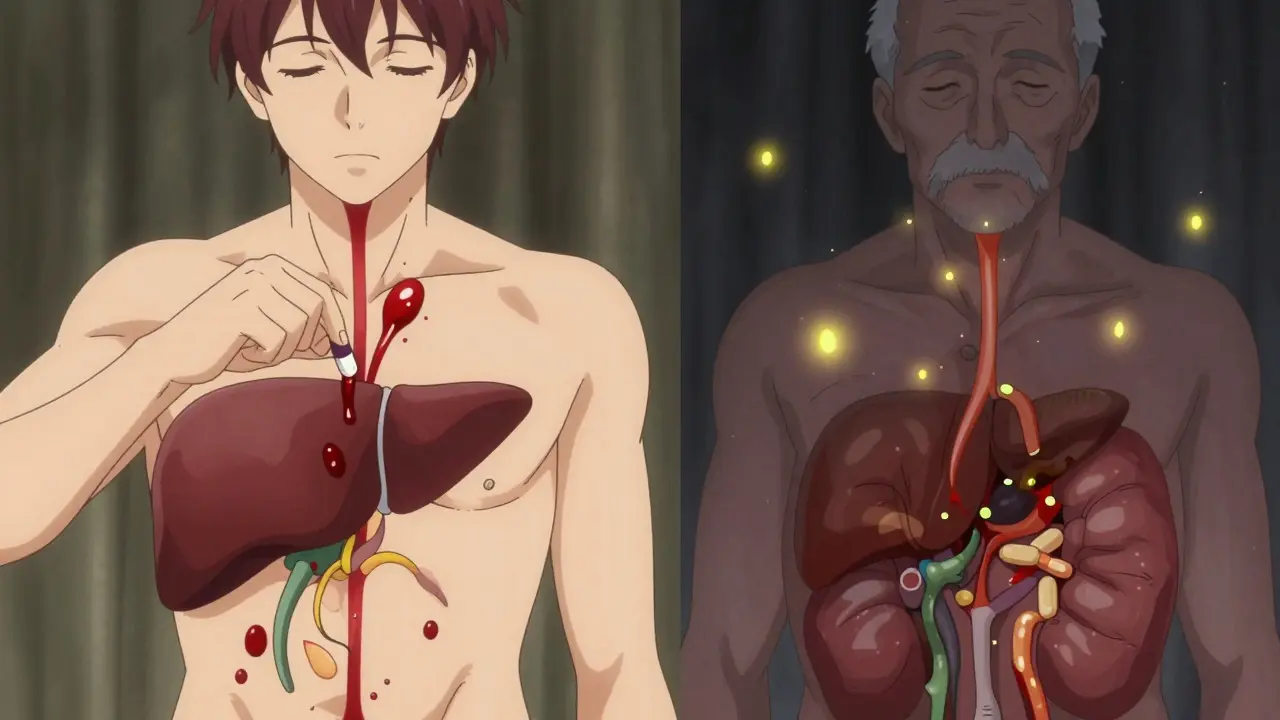
Real-World Consequences: Hospital Beds and Overdoses
This isn’t theoretical. About 10% of hospital admissions in older adults are caused by adverse drug reactions. That’s 1 in 10 seniors admitted to the hospital because a pill they were told to take did more harm than good. One Reddit user, "CaregiverInMA," shared how their 82-year-old mother started on a standard dose of amitriptyline - a common antidepressant - and ended up in the ER with severe dizziness and falls. The dose was fine for a 50-year-old. For her? Too high. Her liver couldn’t clear it. Her kidneys couldn’t help either. After a simple dose reduction, her symptoms vanished. The FDA’s own data shows that 41% of seniors take five or more prescription drugs. That’s a recipe for interactions. A blood pressure pill, a statin, an antidepressant, a painkiller, and a sleep aid - all processed by the same liver enzymes. Add in over-the-counter meds like acetaminophen (Tylenol), and you’ve got a perfect storm. Acetaminophen is responsible for half of all acute liver failures in older adults. Why? Because the liver can’t handle even normal doses when its capacity is already lowered.What Doctors Should Do - And Often Don’t
The American Geriatrics Society has clear guidelines. Start low. Go slow. For drugs processed by the liver, reduce the initial dose by 20-40% in people over 65. For those over 75, go even lower. Use the Cockcroft-Gault equation - or better yet, the CKD-EPI equation - to estimate kidney function. Don’t rely on serum creatinine alone. Always check for drug interactions. A 2020 meta-analysis found that using the STOPP/START criteria (tools that flag inappropriate or missed prescriptions) reduced adverse drug events by 22%. And here’s the hard truth: most clinical trials still don’t include enough older adults. In 2022, only 38% of participants in new drug trials were over 65. So doctors are often guessing. That’s why the FDA now requires drug companies to analyze results by age group - and why tools like GeroDose v2.1 (approved in 2023) are changing the game. This software lets clinicians simulate how a specific person - based on age, weight, liver enzymes, and kidney function - will process a drug.
What You Can Do
If you’re over 65 and taking multiple medications:- Ask your doctor: "Is this dose right for my liver and kidneys?"
- Request a kidney function test using the CKD-EPI formula - not just creatinine.
- Review all your meds - including vitamins, supplements, and OTC painkillers - with your pharmacist.
- Watch for dizziness, confusion, falls, or unusual fatigue. These aren’t "just aging." They might be drug side effects.
- Keep a written list of every pill, patch, or capsule you take. Bring it to every appointment.
The Future: Personalized Dosing
The future of senior medication safety isn’t about age. It’s about biology. Researchers are now identifying epigenetic markers - chemical tags on DNA - that predict how well someone’s liver will metabolize drugs. A 2023 study found 17 methylation sites linked to CYP3A4 activity that change with age. This could lead to blood tests that tell you exactly how your body handles specific drugs. The American Geriatrics Society predicts that by 2030, personalized dosing algorithms - combining genetics, organ function, and drug interactions - could cut adverse drug events in seniors by 35-50%. That’s not science fiction. It’s the next step in medicine.Medication isn’t one-size-fits-all - especially as you age. Your body isn’t broken. It’s just different. And with the right adjustments, you can stay healthy, safe, and in control.
Do all older adults process drugs the same way?
No. While liver and kidney function generally decline with age, the rate varies widely. Genetics, diet, other illnesses, and even gut bacteria affect how drugs are processed. Two 75-year-olds taking the same dose of a medication might have completely different blood levels. That’s why personalized dosing - based on actual organ function - is replacing age-based rules.
Can I still take painkillers like ibuprofen or acetaminophen?
Ibuprofen and other NSAIDs can reduce kidney blood flow and increase the risk of kidney injury in older adults. Acetaminophen (Tylenol) is safer for kidneys but can cause liver damage if taken in doses higher than 3,000 mg per day - even lower if you drink alcohol or have liver disease. Always stick to the lowest effective dose and avoid daily use without doctor approval.
Why do some seniors need lower doses of antidepressants?
Many antidepressants - like amitriptyline, sertraline, and citalopram - are processed by the liver. With reduced liver blood flow and enzyme activity, these drugs build up in the bloodstream. Higher levels increase side effects like dizziness, confusion, and falls. Starting at half the usual dose and increasing slowly is standard practice for older adults.
Should I stop taking my meds if I’m worried about side effects?
Never stop a medication without talking to your doctor. Some drugs - like blood pressure pills or heart medications - can be dangerous to stop suddenly. Instead, write down your symptoms, bring your medication list to your next appointment, and ask: "Could any of these be causing my dizziness or fatigue?"
How often should kidney and liver function be checked in seniors?
At least once a year for healthy seniors. More often - every 3 to 6 months - if you take multiple medications, have diabetes, high blood pressure, or heart disease. Always ask for eGFR (estimated glomerular filtration rate), not just creatinine, to get an accurate picture of kidney function.


This is one of those posts that makes you realize medicine hasn't caught up with real life. I'm 71 and took the same dose of metformin for 10 years until my doc finally checked my eGFR. Turned out I was at 48% and had been quietly accumulating it. No symptoms until I started feeling like I was walking through molasses. Cut the dose by half, and I'm back to hiking weekends. Don't assume 'normal' creatinine means normal kidneys.
Let me tell you something. The entire medical industrial complex is built on ignoring biology. They test drugs on 30-year-old athletes, then sell them to people who can barely climb stairs. And don't get me started on the FDA. They say they 'require age analysis' but 38% of trial participants over 65? That's not inclusion - that's a photo op. I've seen grandmas on 10 meds because their doctor didn't bother to cross-check interactions. It's not negligence. It's negligence with a paycheck.
i had a frined who went to the er after taking tylenol for a week for back pain. they told her it was 'just aging' but no. her liver was fried. she was 72. she didn't even know 3000mg was the limit. her doctor never told her. i mean... how many people are just dying quietly from this? we're being poisoned by our own prescriptions. and the pharma companies? they don't care. they're making bank on people who don't know any better.
What’s wild is how little we talk about the gut-liver-kidney axis in aging. It’s not just organs failing - it’s the ecosystem collapsing. Gut bacteria change with age, and they influence how drugs get metabolized. One study showed that seniors with low microbial diversity had 3x higher levels of certain antidepressants. And we’re still dosing by age instead of microbiome? That’s like giving the same shoe size to everyone because they’re all ‘adults.’ We need personalized maps, not cookie-cutter pills.
This hit home 😭 I’m 68 and my doc finally listened after I said I felt like a zombie. We cut my amitriptyline in half and added a kidney check. Now I’m sleeping better, walking without a cane, and not scared to take a shower alone. You’re not broken. Your body just needs a new map. Thank you for writing this - it’s a lifeline for so many of us.
this is all a lie. the government and big pharma are hiding the truth. they want old people to die so they can save money. the real reason your liver slows down is because of fluoride in the water and 5g cell towers. they don't want you to know. check the patents. they patented the aging process. you're being slowly poisoned. ask your doctor about iodine. it fixes everything.
I just cried reading this. My mom’s in her 80s. She’s been on 8 meds for years. We went in for a routine checkup and the nurse said, 'You know, she’s got the kidneys of a 40-year-old.' We were so relieved... until we found out they’d misread the eGFR. She was actually at 37%. We almost lost her to lithium toxicity. This isn’t science. It’s a minefield. I’m so glad someone finally laid it out like this.
Let’s cut through the fluff. The system is broken. Doctors aren’t villains - they’re drowning in 20-minute appointments and outdated guidelines. But here’s the fix: every senior on polypharmacy should have a pharmacist-led med review every 6 months. Not optional. Mandatory. And we need mandatory geriatric pharmacology in med school. If you can’t pass a 3-hour exam on CYP enzymes and renal clearance, you shouldn’t be writing prescriptions for people over 65. This isn’t radical. It’s basic competence.
As a Canadian geriatric nurse practitioner, I can attest to the profound disconnect between clinical guidelines and real-world practice. The CKD-EPI equation is not merely preferable - it is ethically imperative. Yet, in over 60% of long-term care facilities I’ve consulted, serum creatinine remains the sole metric. This is not an oversight. It is systemic inertia. We must advocate for institutional change, not just individual patient education. The time for incrementalism has passed.
I used to think my dad’s 'confusion' was just dementia. Turns out? It was the leftover hydrocodone from a 2018 back surgery he never stopped taking. We pulled it, switched to acetaminophen at 2g/day, and he’s been his old self for 18 months. Don’t wait for a fall or an ER trip. Sit down with your meds list. Talk to your pharmacist. Ask: 'What if I’m not the 30-year-old they tested this on?' That one question saved my dad’s life.