When cancer is suspected, doctors don’t just guess what’s happening inside the body. They rely on imaging to see exactly where tumors are, how big they are, and whether they’ve spread. The three most important tools for this are PET-CT, MRI, and the newer hybrid PET-MRI. Each one gives different kinds of information, and choosing the right one can change how a patient is treated - or even whether they survive.
What PET-CT Really Shows
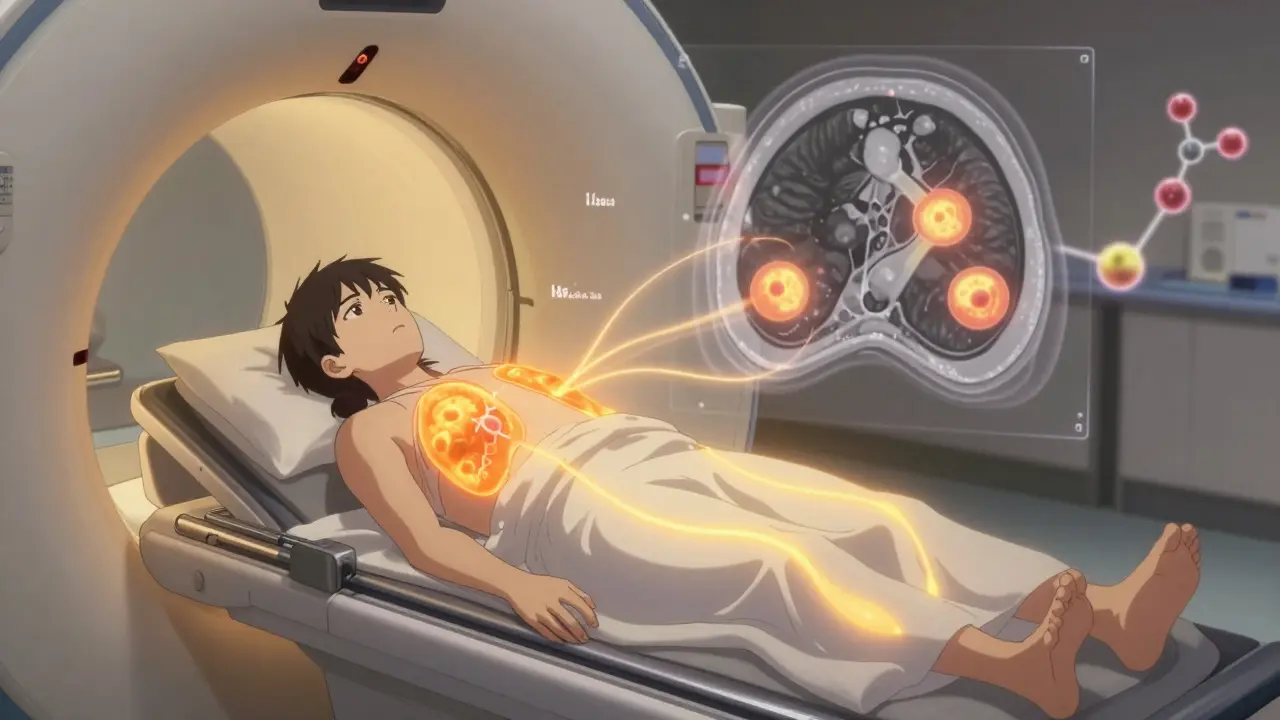
PET-CT combines two scans into one: a PET scan that shows metabolic activity, and a CT scan that maps anatomy. It works because cancer cells burn sugar faster than normal cells. When a patient gets injected with a radioactive sugar tracer - usually 18F-FDG - those cancer cells light up on the scan. The CT part then shows exactly where those glowing spots are in the body.
This combo became the standard in oncology after its FDA approval in 2001. Today, it’s used for nearly every major cancer type: lung, lymphoma, colorectal, melanoma. It’s especially good at spotting distant spread. For example, in non-small cell lung cancer, PET-CT finds metastases in bones or liver that an MRI might miss. A 2023 meta-analysis found it correctly stages 84% of cases.
But it has limits. Not all cancers glow. Some slow-growing tumors, like certain prostate or kidney cancers, don’t take up much of the tracer. And because it uses CT, patients get radiation - typically 10 to 25 mSv per scan. That’s like 3 to 8 years of natural background radiation. For younger patients or those needing repeated scans, that adds up.
MRI: The Soft Tissue Master
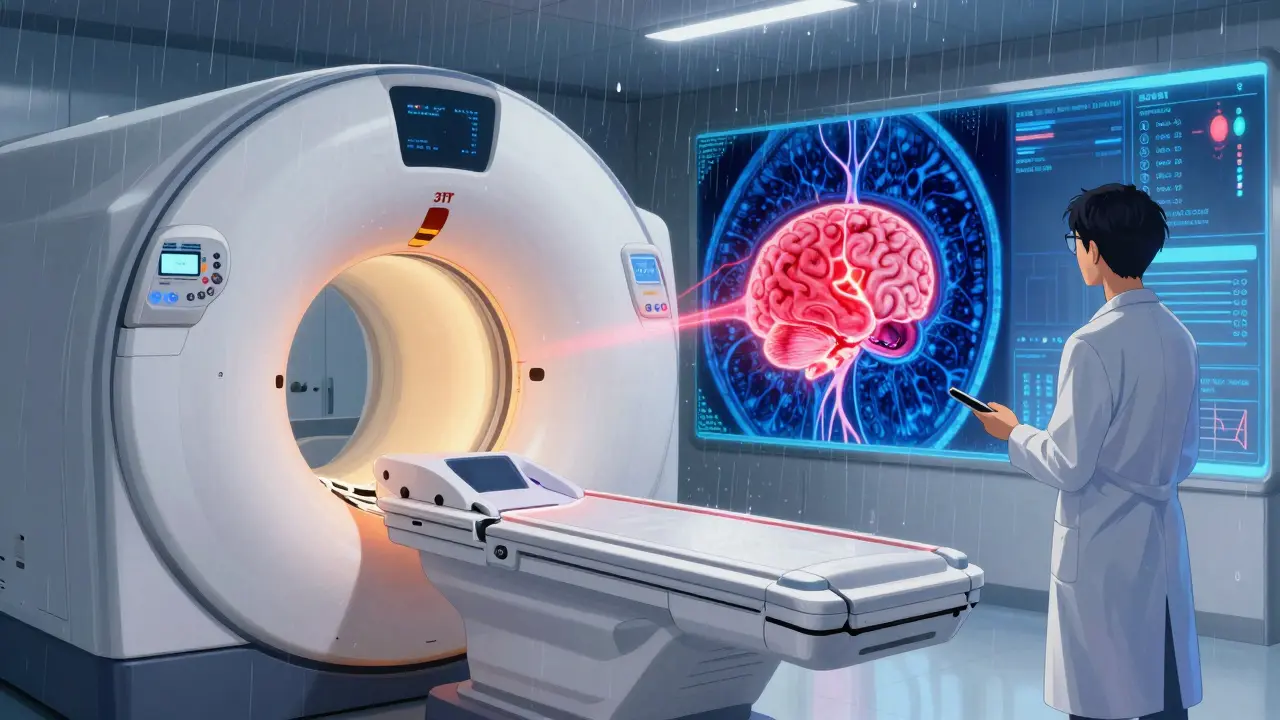
MRI doesn’t use radiation. Instead, it uses powerful magnets and radio waves to create incredibly detailed pictures of soft tissues. That’s why it’s the go-to for brain tumors, spinal cancers, liver lesions, and pelvic cancers like prostate or cervical cancer.
A 3T MRI machine - the most common in hospitals today - can show details as small as half a millimeter. Functional MRI techniques like diffusion-weighted imaging (DWI) can even show how tightly packed cancer cells are, helping tell the difference between scar tissue and active tumor after treatment.
One major advantage? It’s unmatched at spotting recurrence. After radiation therapy, the body often forms scar tissue that looks like a tumor on a CT scan. But MRI can tell them apart. A 2023 review in PMC found MRI alone correctly identified recurrence in 70-80% of brain tumor cases. Add PET to the mix, and that jumps to 85-90%.
Downside? MRI scans take longer - 30 to 60 minutes. Patients have to lie perfectly still. Claustrophobia, metal implants, or even movement from breathing can ruin the images. And while it’s great for local detail, it’s not as good at spotting small tumors far from the main site.
PET-MRI: The Hybrid Advantage
PET-MRI started appearing in major hospitals around 2011. It puts the metabolic power of PET and the soft tissue clarity of MRI into a single machine. You get both types of data in one scan, without needing to move the patient between machines.
This matters most in three areas: brain tumors, pediatric cancers, and pelvic cancers. For kids, reducing radiation is huge. A PET-MRI cuts exposure by about half compared to PET-CT. For prostate cancer, combining PSMA PET with multiparametric MRI can find small tumors that neither scan sees alone. A 2023 study in RadioGraphics found this combo changed treatment plans for nearly half of patients.
But it’s not perfect. The biggest technical headache? Attenuation correction. Because MRI doesn’t measure density like CT does, the PET part can get confused about how much radiation is being absorbed by tissue. This can make tumors look bigger or smaller than they are. Newer systems like Siemens’ BioMatrix 600, cleared in January 2024, use advanced algorithms to fix this, cutting scan time to just 6 minutes for a whole-body scan.
Cost is another issue. A PET-MRI machine costs $3 million to $4.2 million. A PET-CT? Around $2 million. The scan itself can cost $2,500 to $3,500 - 50% more than PET-CT. That’s why most centers only use it for specific cases: when the extra detail will change treatment, or when radiation exposure must be minimized.
Which One Do You Pick?
There’s no single best tool. It depends on the cancer type, location, and what the doctor needs to know.
- For lung cancer or lymphoma: PET-CT is still the standard. It’s fast, widely available, and great at finding spread.
- For brain or spinal tumors: PET-MRI wins. It can tell radiation damage from real tumor regrowth - a life-or-death distinction.
- For prostate cancer: PSMA PET-MRI is becoming the gold standard. It finds tiny tumors that other scans miss.
- For breast cancer after chemo: PET-CT has higher specificity than MRI alone. But for dense breasts, MRI is better at finding residual disease.
- For children or young adults: PET-MRI is preferred whenever possible. Less radiation means less long-term risk.
Even among experts, there’s no universal agreement. Dr. Richard L. Wahl from Johns Hopkins says PET-MRI is best for pelvic and brain cancers, but PET-CT remains the workhorse. Dr. Hedvig Hricak at Memorial Sloan Kettering says the choice must be personalized. And Dr. Barry Siegel points out the cost: if you’re not getting better answers, is it worth the extra $1,000 per scan?
What’s Changing Now?
AI is starting to reshape everything. At the 2023 RSNA meeting, researchers showed AI models that could predict how well a tumor would respond to treatment just from a single PET-MRI scan. These models look at texture, shape, and intensity patterns - things humans can’t see.
Also, new tracers are coming. PSMA for prostate cancer, DOTATATE for neuroendocrine tumors - these are more specific than old FDG tracers. When paired with MRI, they’re turning imaging into a precision tool.
The biggest shift? From “find the tumor” to “understand its behavior.” It’s not just about size anymore. It’s about how aggressive it is, how it’s changing, and whether treatment is working - all before a biopsy or surgery.
Real-World Challenges
Getting these scans isn’t easy. A 2022 survey of 127 radiologists found 73% said PET-MRI’s long scan time slowed down their workflow. Technologists need extra training - at least 40 more hours than for PET-CT. And insurance doesn’t always cover it. Many centers only use PET-MRI for clinical trials or high-risk cases.
Still, adoption is growing. The global PET-MRI market is expected to hit $1.1 billion by 2030. North America leads in usage, but Europe and Asia are catching up fast. Academic hospitals with research programs are the main drivers. Community clinics? They’re still using PET-CT and standard MRI.
One thing’s clear: imaging isn’t just about pictures anymore. It’s about data. And the data from these scans is now guiding personalized treatment plans - not just for diagnosis, but for every step after.
Which imaging test is most accurate for cancer staging?
There’s no single answer. PET-CT is most accurate for cancers that spread widely, like lung or lymphoma. MRI is best for local detail in brain, spine, liver, or pelvic cancers. PET-MRI offers the highest accuracy in specific cases - especially brain tumors and prostate cancer - but it’s not always necessary. The right test depends on cancer type, location, and treatment goals.
Is PET-MRI better than PET-CT for all cancers?
No. PET-MRI is superior for cancers where soft tissue contrast matters - like brain, prostate, liver, or pediatric tumors. But for many cancers, especially those that spread to bones or lungs, PET-CT is faster, cheaper, and just as accurate. Experts agree PET-MRI should be reserved for cases where its added detail will change treatment decisions.
Does MRI detect cancer better than PET-CT?
It depends. MRI detects local tumors better - especially in soft tissues like the prostate or breast. PET-CT is better at finding cancer that has spread to distant organs. In breast cancer, PET-CT is more specific in early response assessment. In prostate cancer, MRI detects more tumors than standard PET-CT, but PSMA PET-CT can outperform MRI in some cases. The best approach often combines both.
How much radiation do these scans expose you to?
A standard PET-CT scan delivers 10-25 mSv of radiation - similar to 3-8 years of natural background radiation. MRI delivers zero radiation. PET-MRI reduces radiation exposure by about 50% compared to PET-CT because it eliminates the CT component’s radiation. This makes PET-MRI especially valuable for children, young adults, and patients needing repeated scans.
Why isn’t PET-MRI used everywhere?
Three main reasons: cost, complexity, and access. A PET-MRI machine costs $3-4.2 million, compared to $1.8-2.5 million for PET-CT. Scans take longer, require specialized training, and many insurance plans don’t cover them unless there’s a clear clinical need. Most hospitals use PET-MRI only for specific cases - like pediatric cancer, recurrent brain tumors, or complex prostate cases - where the extra detail justifies the cost and time.
As cancer care moves toward personalization, imaging is no longer just a picture - it’s a roadmap. The right scan at the right time can mean the difference between starting treatment early or missing a hidden tumor. Knowing which tool does what - and when - helps patients get the care they need without unnecessary risk or cost.


Comments
Post Comment