Most people think of Vitamin D is just a nutrient for strong bones. In reality, it functions more like a secosteroid hormone than a simple vitamin, acting as a master regulator for a vast network of endocrine pathways throughout the body. Because it interacts with receptors in almost every cell type, its influence extends far beyond your skeleton, touching everything from your immune response to your blood pressure.
The Biological Journey: From Sunlight to Hormone
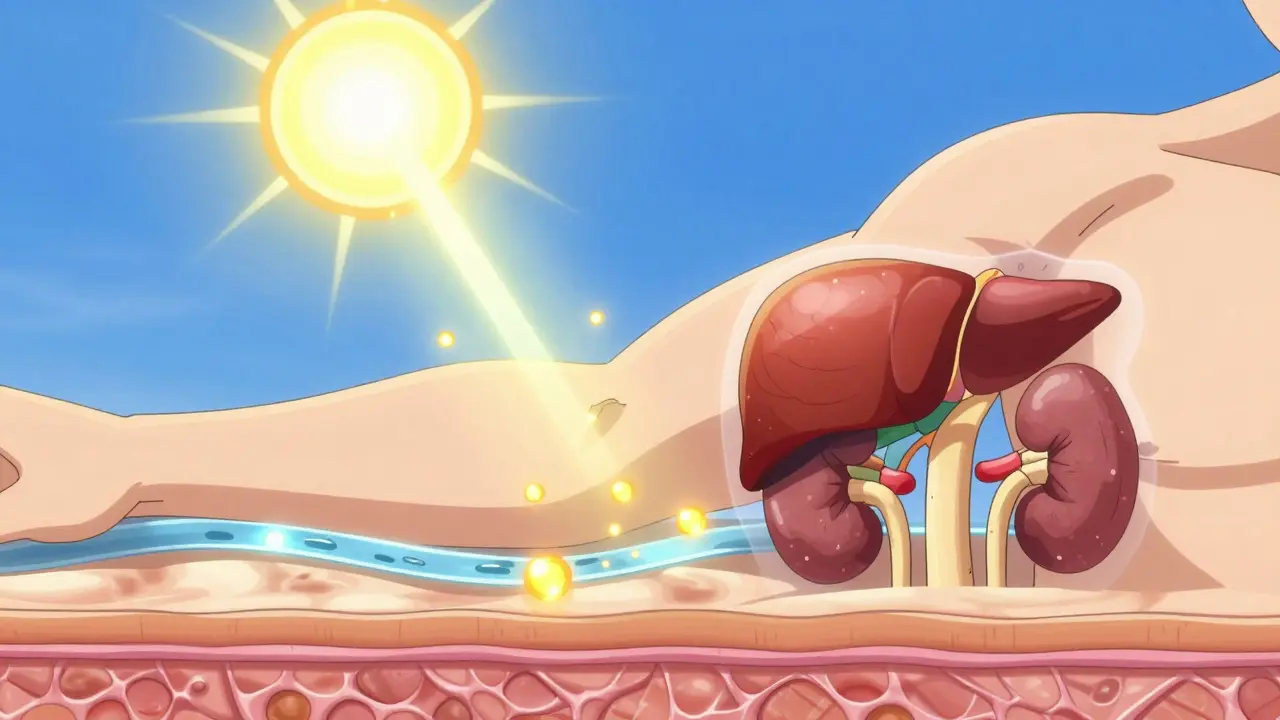
To understand how Vitamin D affects your endocrine system, you first have to look at how your body processes it. It isn't active the moment you get it from the sun or a supplement. It requires a two-step chemical transformation to become biologically useful.
First, your skin synthesizes Vitamin D3 (cholecalciferol) when exposed to UVB rays. This D3, or the Vitamin D2 (ergocalciferol) you get from plants, travels to the liver. There, an enzyme called CYP2R1 converts it into 25-hydroxyvitamin D, also known as 25(OH)D. This is the form doctors measure in blood tests to determine if you are deficient.
The final step happens in the kidneys. An enzyme called CYP27B1 converts 25(OH)D into calcitriol (1,25-dihydroxyvitamin D). This is the truly active hormone. This process is tightly managed by the Parathyroid Hormone (PTH) and phosphorus levels to ensure your blood calcium remains in a narrow, healthy range between 8.5 and 10.5 mg/dL.
How Vitamin D Controls Your Genes
The real magic happens at the cellular level via the Vitamin D Receptor (VDR). Think of the VDR as a lock, and calcitriol as the key. When the key turns the lock, it triggers changes in how your DNA is read. Research shows that the VDR can regulate over 11,000 different target genes.
These genes aren't just for bone growth. They fall into several critical categories: about 43% are involved in metabolism, while others control cell morphology, tissue adhesion, and even the growth of new blood vessels (angiogenesis). This explains why vitamin D is linked to so many different organ systems. If your VDR isn't activated, these genetic instructions aren't delivered, which can lead to a cascade of endocrine imbalances.
Endocrine vs. Autocrine: The Great Paradox
There is a confusing gap between what a blood test says and how your body actually feels. This is because vitamin D works in two different ways: the systemic (endocrine) pathway and the local (autocrine) pathway.
- The Endocrine Pathway: This is the "classic" route. The kidneys produce calcitriol, which enters the bloodstream to tell the intestines to absorb more calcium and the bones to release calcium if levels are too low. This is a global system designed to keep your heart and muscles working.
- The Autocrine Pathway: This is a local operation. Many tissues, like immune cells and pancreatic beta cells, have their own CYP27B1 enzymes. They can convert vitamin D into its active form right there on the spot, even if your overall blood levels aren't skyrocketing.
This distinction is why some people feel a "dramatic improvement" in fatigue and muscle strength after supplementing, while others see their blood levels rise without feeling any different. Your blood test measures the 25(OH)D storage tank, but it doesn't tell you if your immune cells are actually producing the active hormone they need.
| Feature | Endocrine Pathway | Autocrine Pathway |
|---|---|---|
| Primary Site | Kidneys (Systemic) | Local Tissues (e.g., Macrophages) |
| Main Goal | Blood Calcium Homeostasis | Local Gene Regulation |
| Regulation | Strictly controlled by PTH | Independent of PTH |
| Blood Marker | Correlates with 25(OH)D | Often independent of serum levels |

Navigating Supplementation and Dosages
If you're looking to optimize your Vitamin D levels, one size definitely does not fit all. The standard recommendation for most adults is 600 to 2,000 IU per day. However, your specific biology changes the math.
For instance, if you have a BMI over 30, you might need 2 to 3 times the standard dose. This is because vitamin D is fat-soluble; it gets sequestered in adipose tissue, meaning there is less available in your bloodstream. Similarly, people with celiac disease or other malabsorption syndromes often need significantly higher doses, sometimes as much as 50,000 IU weekly for a short period, to overcome the gut's inability to absorb the nutrient.
But be careful with "mega-dosing." Taking more than 4,000 IU daily without supervision can increase the risk of hypercalcemia (too much calcium in the blood). Toxicity usually doesn't kick in until blood levels exceed 150 ng/mL, but individual sensitivity varies based on your genetics-specifically polymorphisms in your vitamin D binding protein (DBP).
The Controversy: Bone Health vs. Disease Prevention
You'll find a huge divide in the medical community regarding whether vitamin D prevents chronic diseases. On one side, experts like Dr. Michael Holick argue that deficiency is a root cause for type 2 diabetes and cardiovascular disease, pointing to data that shows a 30-50% higher risk in those with low levels.
On the other side, large-scale trials like the VITAL study found that 2,000 IU per day didn't actually reduce the incidence of major heart events or invasive cancers in a general population. This creates a paradox: the lab data looks amazing, but the real-world population results are mixed. The likely reason is that many people in these trials weren't actually deficient, so the supplements provided no added benefit.
Practical Tips for Managing Your Levels
If you're tracking your health, keep these rules of thumb in mind:
- Wait to Retest: Your blood levels lag behind your supplementation. If you start a new dose today, don't retest for 2 to 3 months. Testing too early will give you a false reading.
- Check Your Risk Group: If you have chronic kidney disease or osteoporosis, you are at a much higher risk (up to 70% deficiency in some kidney stages) and should be monitored closely.
- Pair with Fat: Since vitamin D is fat-soluble, taking your supplement with a meal containing healthy fats improves absorption.
What is a "sufficient" level of Vitamin D?
The Endocrine Society considers 30-100 ng/mL to be sufficient. However, some health organizations, like the Institute of Medicine, argue that 20 ng/mL is enough for most of the population. Most clinicians aim for at least 30 ng/mL to ensure optimal bone and immune health.
Can I take too much Vitamin D?
Yes. While rare, extremely high doses can lead to toxicity, characterized by hypercalcemia. This usually happens when serum 25(OH)D levels exceed 150 ng/mL, leading to calcium buildup in the blood and soft tissues.
Why doesn't my supplement seem to be working?
It could be a few things. You might have a malabsorption issue (like celiac disease), or you may have a genetic variation in the CYP2R1 enzyme that affects how you process the vitamin. Additionally, if you have a high BMI, the vitamin may be stored in fat cells rather than circulating in your blood.
What is the difference between D2 and D3?
Vitamin D2 (ergocalciferol) comes from plant sources and fungi. Vitamin D3 (cholecalciferol) is synthesized by your skin from sunlight or found in animal products. D3 is generally considered more effective at raising and maintaining blood levels of 25(OH)D.
Do I really need a blood test to start supplements?
For most healthy adults, a moderate dose (600-2,000 IU) is safe without a test. However, if you have high-risk factors-such as kidney disease, osteoporosis, or obesity-a baseline test is critical to avoid under-dosing or toxicity.
Next Steps for Different Needs
If you are a healthy adult with a standard diet, focusing on safe sun exposure and a moderate supplement is usually enough. However, if you have a diagnosed endocrine disorder, your path is different. Those with chronic kidney disease should work with a specialist to use specific analogs like paricalcitol, which can lower parathyroid hormone levels without causing the dangerous calcium spikes associated with standard vitamin D.
For those struggling with obesity, the strategy is "weight-adjusted dosing." Instead of the standard 800 IU, you may need to aim for 3,000 IU to reach that 30 ng/mL goal. Always monitor your levels every three months when adjusting high doses until you hit a stable maintenance level.


The distinction between endocrine and autocrine pathways is fundamental, yet most of the lay public remains blissfully ignorant of the nuance. It is quite amusing that people obsess over their serum 25(OH)D levels while completely ignoring the role of local CYP27B1 enzymes in the macrophages. One would think that the concept of cellular autonomy in hormone conversion would be intuitive to anyone with a basic understanding of biochemistry, but alas, we are left with a population that views a blood test as an absolute truth rather than a systemic snapshot. The reality is that your systemic levels are merely a proxy for potential, not a guarantee of local activity. Without considering the VDR polymorphism, these discussions on 'optimal' levels are essentially academic exercises in guesswork. It is high time we moved beyond the simplistic 'deficiency vs. sufficiency' binary and started discussing the actual kinetics of the secosteroid hormone system properly.