Celiac Disease: What It Is, How to Spot It, and Easy Ways to Feel Better
If you’ve ever felt bloated after a slice of pizza or got weird skin rashes for no clear reason, celiac disease might be lurking. It’s not just a food dislike – it’s an autoimmune reaction that attacks your gut when you eat gluten. Gluten is the protein found in wheat, barley and rye, so even tiny crumbs can set off trouble.
Most people think of stomach pain, but celiac shows up in many ways: constant fatigue, anemia, joint aches, or even mood swings. Kids might struggle with growth, while adults could notice unexplained weight loss. The key is that symptoms vary a lot, which is why it’s easy to miss.
How Doctors Figure Out If It’s Celiac
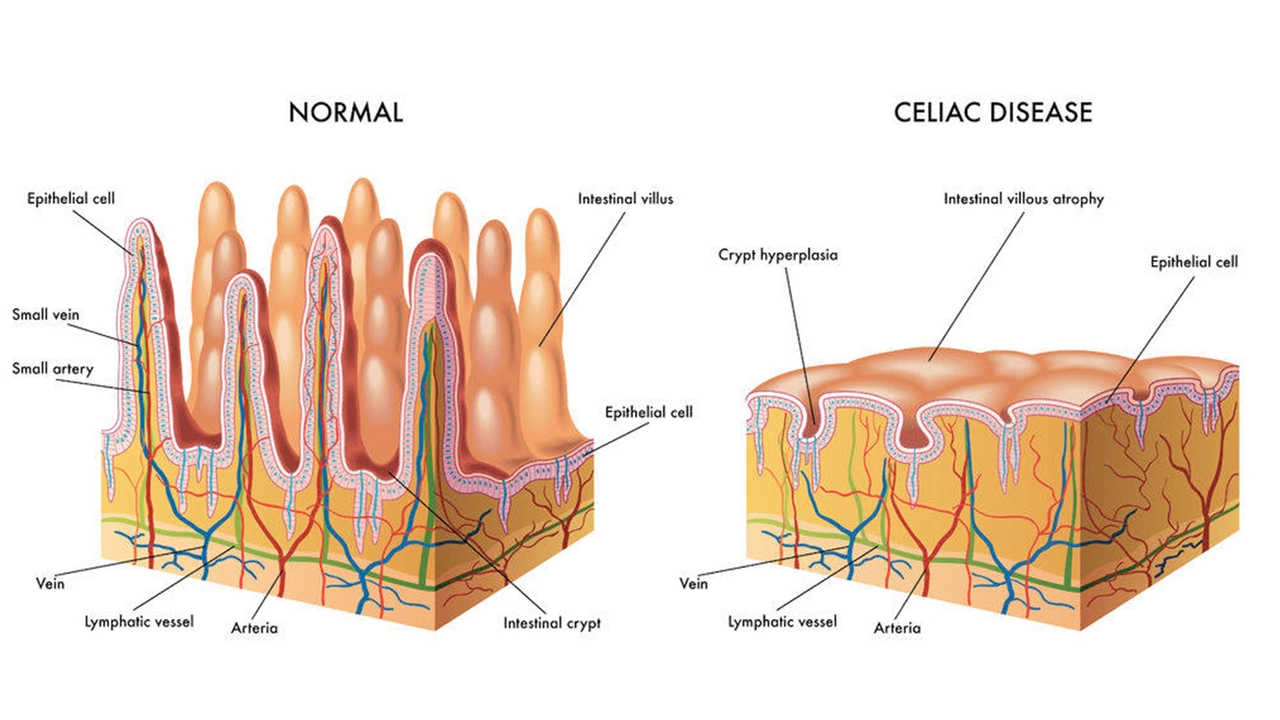
The first step is usually a blood test looking for specific antibodies (tTG‑IgA is the most common). If those are high, doctors will suggest an endoscopy where they take tiny samples from your small intestine. Those biopsies reveal if the lining is damaged – the hallmark of celiac.
It’s super important not to quit gluten before testing. Even a few days off can lower antibody levels and give a false‑negative result. If you suspect celiac, keep eating normally until you see a doctor.
Living Gluten‑Free Without Losing Your Mind
The biggest change is cutting out anything with wheat, barley or rye. That means saying goodbye to regular bread, pasta and most baked goods – unless they’re specially labeled gluten‑free. Look for the “gluten‑free” seal on packages; it’s a quick way to stay safe.
Stock your pantry with naturally gluten‑free foods: rice, potatoes, quinoa, corn, beans, fresh fruits and veggies, nuts, seeds, and most dairy products. Gluten‑free flours (like almond or coconut) let you bake at home without the mystery of hidden wheat.
Dining out can feel tricky, but many restaurants now have dedicated gluten‑free menus. Always tell your server about your celiac – they can often take extra steps to avoid cross‑contamination.
Watch for hidden gluten in sauces, soups and processed meats. A splash of soy sauce or a pre‑made gravy could ruin your day. Reading ingredient lists is the safest habit you’ll develop.
If you’re worried about missing nutrients, especially iron, calcium and B vitamins, consider a multivitamin or talk to a dietitian. They can help you create balanced meals that keep you strong while staying gluten‑free.
Living with celiac isn’t a punishment; it’s a chance to explore new foods and healthier habits. Many people report feeling more energetic, clearer skin and better digestion once they stick to the plan.
Bottom line: if you have persistent gut issues or odd symptoms, get tested before you change your diet. A proper diagnosis lets you tackle celiac the right way, and a simple gluten‑free switch can make a huge difference in how you feel day to day.
In my latest research, I delved into the relationship between Aspirin and celiac disease, particularly its safety for those with gluten sensitivities. It appears that Aspirin, like many medications, can contain gluten, posing a risk for those with celiac disease. However, many manufacturers are now producing gluten-free versions. It's crucial to always check the labels or consult a healthcare professional before use. Remember, vigilance and awareness are key in managing celiac disease.