
Every year, tens of thousands of people in the U.S. get bitten by a tick and never think twice about it. But for some, that tiny bite turns into something far more serious - Lyme disease. It’s not just a summer nuisance. It’s a bacterial infection that can creep through your body, hiding in joints, nerves, and even your heart. And if you don’t catch it early, it can turn into a long, painful battle. The good news? If you know the signs and act fast, you can beat it. The bad news? Many people don’t recognize it until it’s too late.
How Lyme Disease Starts - And Why Timing Matters
Lyme disease is caused by a spiral-shaped bacterium called Borrelia burgdorferi a spirochete bacterium transmitted by infected blacklegged ticks. It’s not spread by all ticks - only specific ones. In the U.S., two species are the main culprits: Ixodes scapularis the blacklegged tick, common in the Northeast and Midwest and Ixodes pacificus the Western blacklegged tick, found along the Pacific coast. These ticks don’t jump or fly. They wait on grass or brush, latch onto you as you walk by, and then feed.Here’s the scary part: the tick has to be attached for at least 24 hours to pass the bacteria. Some research says transmission can start as early as 15 hours, but the CDC says 24 hours is the safe threshold. That’s why checking yourself after being outdoors - especially in wooded or grassy areas - is critical. Nymph ticks, the size of a poppy seed, are the biggest threat. They’re hard to spot, and they’re most active in spring and summer, right when people are hiking, camping, or gardening.
Once the tick bites, the bacteria move from its gut into your bloodstream. It takes time. That’s why symptoms don’t show up right away. You might not feel anything for days, even weeks. But when they do, they come in stages.
The Three Stages of Lyme Disease - And What Happens in Each
Lyme disease doesn’t hit you all at once. It unfolds in three phases - and each one has different symptoms and treatment needs.
Stage 1: Early Localized (1-28 days after bite)
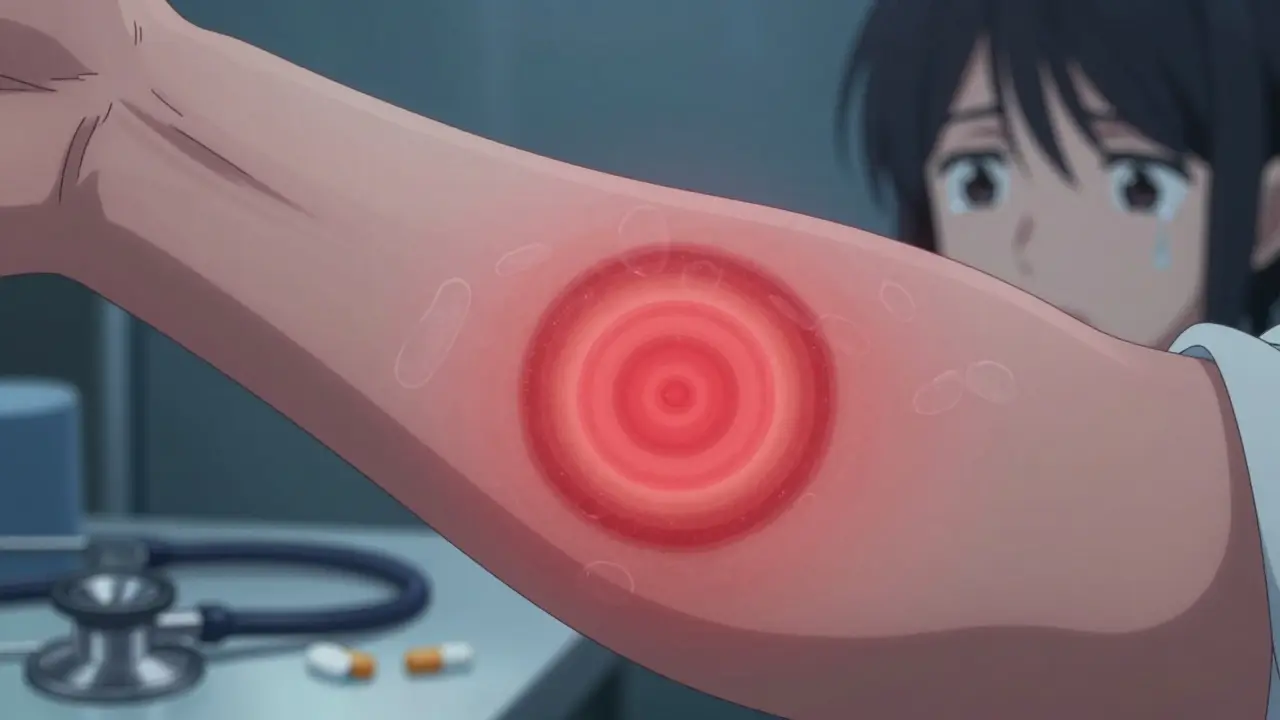
This is the window where you still have the best chance to stop it cold. About 70-80% of infected people develop a rash called erythema migrans a circular, expanding red rash that often looks like a bull’s-eye. It usually shows up 7-14 days after the bite. The rash isn’t itchy or painful, but it keeps growing - sometimes over several inches. It can appear anywhere: your thigh, back, armpit, even your scalp.
Along with the rash, you might feel flu-like symptoms: fever (45% of cases), chills, fatigue (70%), headache (61%), and muscle aches. These aren’t unique to Lyme, so many people think they’ve just got a bad cold. But if you’ve been in a tick-heavy area and have this rash? That’s your red flag. Dr. Allen Steere, who first identified Lyme disease in the 1970s, says the rash alone is enough to diagnose Lyme - no lab test needed.
At this stage, treatment is simple. A 10-21 day course of oral antibiotics - usually doxycycline a tetracycline antibiotic effective against Borrelia burgdorferi for adults or amoxicillin a penicillin-class antibiotic used for children and pregnant women for kids - clears the infection in over 90% of cases. The CDC reports that 87% of patients treated within 30 days of symptoms fully recover within three months.
Stage 2: Early Disseminated (weeks to months after bite)
If you miss Stage 1, the bacteria start spreading. This is where things get complicated. Weeks or even months later, you might develop multiple rashes, or the infection moves to your nervous system or heart.
Neurological symptoms can include facial palsy loss of muscle tone on one or both sides of the face, often mistaken for a stroke. It happens in 5-10% of untreated cases. You might also get severe headaches, neck stiffness, or tingling in your hands and feet. Some people develop Lyme carditis inflammation of the heart tissue that can cause irregular heartbeat, which affects 4-10% of untreated patients. In rare cases, the heart’s electrical signals get disrupted, leading to fainting or dizziness.
Treatment now gets more intense. You’ll likely need 14-28 days of intravenous antibiotics such as ceftriaxone, delivered directly into the bloodstream. This isn’t a simple pill anymore. You’ll need a clinic visit or home IV therapy. But even then, recovery isn’t guaranteed. Some people still end up with lingering symptoms.
Stage 3: Late Disseminated (months to years after bite)
This is what happens when Lyme is ignored for too long. Without treatment, about 60% of people develop intermittent arthritis severe joint pain and swelling, especially in the knees. It comes and goes, sometimes for years. Other long-term issues include nerve pain, brain fog, memory loss, and trouble concentrating.
These symptoms are often mistaken for autoimmune diseases like multiple sclerosis or fibromyalgia. That’s why many patients see 3 or more doctors before getting the right diagnosis. One Reddit user, who posted under the name “LymeWarrior2020,” spent 18 months and visited seven doctors before finally being diagnosed with neurological Lyme disease. By then, the damage was already done.
Why Diagnosis Is So Hard - And What’s Changing
Testing for Lyme disease isn’t foolproof. The standard two-tier blood test - ELISA followed by Western blot - only catches about 30% of cases in the first few weeks. Why? Because your body hasn’t made enough antibodies yet. A 2023 study in Emerging Infectious Diseases found that current tests miss 35% of early Lyme cases.
That’s why doctors are taught to rely on symptoms first - especially the rash. If you have the bull’s-eye, treat it. Don’t wait for a lab result. But many primary care providers still don’t know this. A 2022 study found only 52% of them could correctly identify all three stages of Lyme disease in a clinical scenario.
Good news: in March 2023, the FDA approved the first new Lyme diagnostic test in 20 years - the MiQLick test a urine-based test detecting Borrelia burgdorferi DNA with 92% sensitivity. It’s not widely available yet, but it’s a step toward faster, more accurate detection. Researchers are also working on an mRNA vaccine, expected to enter human trials in mid-2024.

The Controversy: Chronic Lyme vs. Post-Treatment Lyme Disease Syndrome
This is where things get messy. Some patients - about 10-20% - keep feeling tired, achy, or foggy even after finishing antibiotics. The medical community calls this Post-Treatment Lyme Disease Syndrome (PTLDS) persistent symptoms lasting over six months after standard treatment. It’s not an active infection. It’s likely your immune system is still reacting to past damage.
But not everyone agrees. Groups like the International Lyme and Associated Diseases Society (ILADS) argue that long-term antibiotics can help. The Infectious Diseases Society of America (IDSA) says there’s no proof. And in 28 states, doctors are legally protected for prescribing months of antibiotics - even though major medical groups warn it doesn’t work and can cause harm.
Dr. John Aucott from Johns Hopkins has studied PTLDS for years. He says it’s real, but it’s not caused by lingering bacteria. It’s like a fire that burned out - but the smoke still lingers. Recovery takes time. Physical therapy, sleep support, and stress management help more than more antibiotics.
What You Can Do - Prevention and Action Steps
Here’s the bottom line: Lyme is preventable. And treatable - if you catch it early.
- After being outdoors - especially in tick country - check your whole body. Don’t skip behind the ears, under the arms, or between your toes.
- Shower within two hours of coming inside. It helps wash off unattached ticks.
- If you find a tick, remove it with fine-tipped tweezers. Pull straight up. Don’t twist. Save it in a baggie if you can.
- If you’re in a high-risk area (Minnesota, Wisconsin, Pennsylvania, etc.) and the tick was attached for over 36 hours, ask your doctor about a single 200mg dose of doxycycline within 72 hours. It cuts infection risk by 95%.
- Don’t wait for a rash to appear. If you’ve been bitten and feel off, get checked.
The CDC estimates 476,000 people get Lyme every year - but only 30,000 are officially reported. That gap exists because many cases go undiagnosed. You can change that. Know the signs. Act fast. And don’t let confusion stop you from getting help.
Can you get Lyme disease from a dog or cat?
No. Dogs and cats can get Lyme disease, but they can’t pass it to humans. The only way you get Lyme is through the bite of an infected tick. However, if your pet has ticks, they can bring them into your home. Check your pets after they’ve been outside, especially in wooded areas.
Is the Lyme disease rash always a bull’s-eye?
No. While the classic bull’s-eye pattern is common, about 20-30% of rashes are solid red or have irregular shapes. Don’t wait for the perfect ring. If you see a spreading red patch after a tick bite, get it checked.
Can you get Lyme disease more than once?
Yes. Getting Lyme once doesn’t make you immune. You can be bitten again - even in the same year. That’s why ongoing prevention matters, even if you’ve had it before.
Do tick repellents work?
Yes. Products with DEET (20-30%), picaridin, or permethrin-treated clothing reduce tick bites by up to 80%. Apply repellent to skin and clothes. Permethrin on gear lasts through several washes. It’s one of the most effective ways to prevent exposure.
What if I live outside the high-risk states?
Lyme is spreading. Climate change is pushing ticks north and west. Cases have been reported in all 50 states. Even if you’re not in a known hotspot, if you’re spending time outdoors - especially in grass, brush, or woods - you’re at risk. Stay vigilant.



I've seen this in my ER rotations. The bullseye rash is rare. More often it's just a red patch that fades. People panic when they don't see the perfect ring. If you've been in the woods and feel off, get treated. Don't wait for a test. The CDC's 24-hour rule is conservative. I've seen transmission at 18 hours. Time is tissue.
I got bit in Vermont last year and ignored it. Thought it was just a bug bite. Then I woke up with my face drooping. Went to three doctors before someone said 'Lyme'. They gave me IV antibiotics for 21 days. Still get brain fog sometimes. I'm not one of those 'chronic Lyme' people but I do think we're underestimating how long recovery takes. Your body doesn't just reset after antibiotics. It takes months of rest, sleep, and zero stress. I wish I'd known that sooner. Now I tell everyone to check themselves after hiking. Even if they don't see a tick. Even if they don't feel anything. Just check.
I find it astonishing that the medical establishment still relies on antiquated serological tests when molecular diagnostics have been available for over a decade. The MiQLick test, as referenced, represents a paradigm shift; however, its adoption is hindered by institutional inertia and pharmaceutical lobbying. Furthermore, the notion that Lyme disease cannot persist beyond standard antibiotic regimens is not only scientifically unsound but also ethically indefensible. One must question the integrity of organizations that dismiss patient-reported outcomes as psychosomatic.
The assertion that 'treatment is simple' in Stage 1 is dangerously misleading. Doxycycline is not a panacea. It suppresses, it does not eradicate. The spirochete's ability to form biofilms and cystic forms is well-documented in peer-reviewed literature. To claim 90% recovery is to ignore the growing body of evidence indicating persistent infection. I have colleagues who have treated hundreds of patients with long-term antimicrobial protocols - and they report significant improvement. This is not fringe medicine. It is medicine that has been silenced.
So let me get this straight. You're telling me that if I get bit by a tick and I don't have the perfect bullseye rash, I should just go ahead and take antibiotics? What about the rise in antibiotic resistance? What about the microbiome? What about the fact that 30% of ticks in some areas aren't even infected? This is fearmongering dressed up as public health advice. People are getting scared into overmedicating themselves. That's not prevention. That's panic.
You're right to worry about overuse. But in high-risk areas with confirmed tick exposure, the risk-benefit is clear. A single 200mg dose of doxycycline has a 95% success rate at preventing infection. That's better than most vaccines. And it's not long-term. It's one pill. You're not killing your microbiome. You're stopping a disease that can cripple you. Don't let perfect be the enemy of good.
I work in a clinic in Maine. We see 30+ cases a month. Most people come in late. They say 'I felt fine for weeks'. Then they get joint pain. Or dizziness. Or their heart skips. We give them the 10-day course. 8 out of 10 get better. The rest? They need more. But we don't just throw antibiotics at them. We check thyroid. We check vitamin D. We check sleep. Lyme isn't the only thing that makes you tired. You gotta rule out the basics first.
Coming from India, I never thought ticks were a big deal here. But after reading this, I realize my cousin in Minnesota had Lyme and no one knew. It took her 6 months to get diagnosed. I now tell everyone: if you go hiking, wear permethrin-treated clothes. It's cheap. It lasts. And it works. Also, check your pets. They bring ticks inside. My dog brought in three last summer. One was a nymph. I almost missed it. Scary stuff. But preventable.
They're hiding the truth. The CDC knows ticks are genetically modified. The government is testing bio-weapons in national parks. That's why Lyme is spreading so fast. They don't want you to know. The MiQLick test? It's a distraction. Real doctors know the truth: Lyme is part of a larger agenda. Vaccines? They're not for you. They're for control. I've been studying this for 12 years. The signs are everywhere. Why do you think they call it 'Post-Treatment Syndrome'? Because they don't want to admit they can't cure it. They're covering up.
The notion that Lyme disease is merely a bacterial infection is a gross oversimplification. The spirochete, Borrelia burgdorferi, exhibits extraordinary phenotypic plasticity, including the formation of persister cells and biofilm-like aggregates. To suggest that a 21-day course of antibiotics constitutes a 'cure' is not only scientifically indefensible but a disservice to patients who suffer from persistent multisystemic dysfunction. The medical establishment's refusal to acknowledge this constitutes malpractice. The FDA's approval of the MiQLick test is a step forward - but insufficient. We require longitudinal studies, not siloed diagnostics.
I'm a lab tech. We run the ELISA/Western blot tests daily. They're garbage in the first 30 days. I've seen patients with clear rashes and negative tests. We treat anyway. The system is broken. The CDC guidelines are outdated. We need better tools. And we need to stop pretending that every symptom after treatment is 'PTLDS'. Some people have lingering infection. We just don't have the tech to prove it yet.